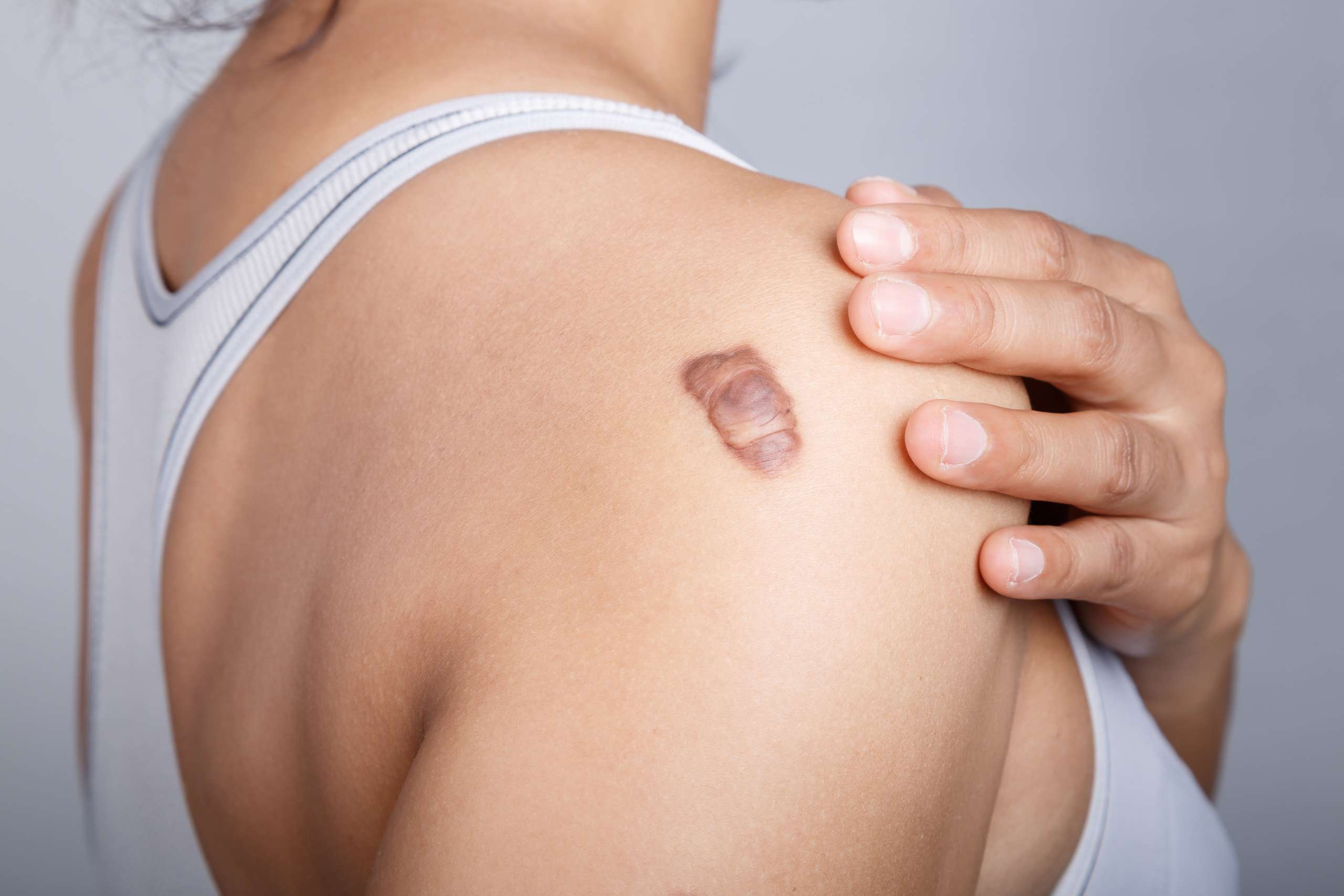
At DermDox, we understand the physical and emotional impact that keloids can have on individuals. Keloids are thick, raised, and often itchy scars that extend beyond the boundaries of the original wound, resulting from an overgrowth of collagen during the healing process. Our dedicated team of dermatologists specializes in providing advanced and personalized keloid treatments to help patients regain confidence in their skin. DermDox offers cutting-edge solutions designed to effectively reduce the appearance of keloids, alleviate discomfort, and prevent their recurrence.
Our approach to keloid treatment at DermDox is tailored to each patient’s unique needs. We employ a combination of therapies, including corticosteroid injections, laser therapy, cryotherapy, and silicone sheets or gels, to flatten and soften the keloid tissue. In some cases, surgical excision or laser therapy is used to remove the keloid, followed by preventive measures to minimize the risk of recurrence. With a focus on patient care, DermDox dermatologists collaborate closely with individuals to create customized treatment plans. By providing compassionate and comprehensive keloid treatments, DermDox aims to enhance the overall well-being of patients, empowering them to feel more comfortable and confident in their skin.
Frequently Asked Questions
Keloids develop when the body’s natural healing process goes awry, leading to an overproduction of collagen at the site of a wound or injury. While the exact cause of keloids is not fully understood, several factors can contribute to their formation:
Genetic Predisposition: Genetic factors play a significant role in keloid formation. Individuals with a family history of keloids are more likely to develop them, suggesting a genetic predisposition to this condition.
Skin Type: People with darker skin tones, particularly those of African, Asian, or Hispanic descent, are more prone to keloid formation. Darker skin types have a higher melanin content, and melanocytes (pigment-producing cells) may influence the body’s response to injury and wound healing.
Wound or Injury Severity: Keloids often develop after injuries or wounds that penetrate deep into the skin layers, such as surgical incisions, severe burns, acne scars, or ear piercings. The risk increases with more significant injuries or surgeries.
Age and Hormonal Influence: Keloids are more common in young individuals, particularly during adolescence and early adulthood. Hormonal changes during puberty and pregnancy might influence keloid formation.
Inflammatory Response: An exaggerated inflammatory response at the site of injury can contribute to keloid development. Individuals with an overly active immune system or chronic inflammation may be more susceptible.
Tension on the Skin: Constant tension or pulling on the skin, such as in areas prone to repetitive motion or joint movement, can increase the risk of keloids. Tight clothing, body piercings, or certain hairstyles may contribute to keloid formation.
It’s important to note that not everyone with these risk factors will develop keloids, and the exact reasons why some individuals are more prone to keloid formation remain a subject of ongoing research. While keloids are generally harmless, they can cause discomfort, itching, or self-consciousness about their appearance.
Keloids are typically persistent and often do not go away on their own. Once formed, keloids tend to remain unless treated. However, they may sometimes become less noticeable or flatten slightly over time, but they usually do not disappear completely without intervention.
Various treatment options are available to manage keloids and reduce their size, thickness, and discomfort. These treatments aim to improve the appearance of keloids and alleviate symptoms. Common keloid treatments include corticosteroid injections, laser therapy, cryotherapy (freezing the keloid with liquid nitrogen), silicone sheets or gels, pressure dressings, and surgical excision. In some cases, a combination of these treatments may be used for optimal results.
It’s important to note that keloid treatment outcomes vary from person to person. While some individuals respond well to treatments and experience significant improvement, others may have a limited response. Additionally, keloids have a tendency to recur, even after successful treatment, making it essential for individuals to follow up with their healthcare provider for ongoing management and preventive measures.
If you develop a keloid around a piercing, it’s advisable to consult a healthcare professional, preferably a dermatologist, for proper evaluation and guidance. The decision to remove the piercing should be made in consultation with a medical professional who can assess the keloid’s severity, size, and location.
In some cases, removing the piercing might be recommended, especially if the keloid is causing discomfort, pain, or if the piercing site shows signs of infection. Removing the source of irritation (the piercing) can sometimes prevent the keloid from growing larger or becoming more problematic.
If a keloid appears to have ruptured or popped, it’s important to seek medical attention promptly. While keloids don’t contain pus like some types of cysts or abscesses, a keloid that has broken open can be vulnerable to infection, which may lead to complications.
Here’s what can happen if a keloid pops:
Risk of Infection: When a keloid ruptures, it exposes the underlying tissue to bacteria. This can lead to an infection in the area, causing redness, swelling, warmth, pain, and potentially producing pus. Infections require medical treatment, usually with antibiotics.
Potential for Enlargement: Contrary to common belief, keloids don’t always shrink after they rupture. In some cases, especially if an infection develops, the keloid might continue to grow, becoming even larger than before.
Increased Discomfort: Ruptured keloids can be painful, and the open wound can cause discomfort, especially if it’s located in an area prone to movement or friction, such as joints or under tight clothing.
Scarring: Healing from a ruptured keloid can result in further scarring, potentially leading to a larger or more prominent keloid in the long run.
If you suspect that your keloid has ruptured or if you’re experiencing signs of infection around the area, it’s crucial to consult a healthcare professional, preferably a dermatologist or a healthcare provider experienced in keloid management. They can assess the situation, provide appropriate wound care, and, if necessary, prescribe antibiotics to prevent or treat infection. It’s important to avoid squeezing, poking, or attempting to drain the keloid yourself, as this can worsen the situation and increase the risk of infection.